
What Does It Mean To Be a Midwife?
There’s a global need for 1.1 million more sexual, reproductive, maternal, newborn and adolescent health (SRMNAH) workers, mostly midwives in Africa. Learn more about the essential role of midwives in Sierra Leone in this Q&A with Project HOPE newborn consultant Banneh Daramy.
The COVID-19 pandemic illuminated the vital role midwives play in protecting the lives of women and children around the world — and the importance of investing in them.
The world is facing a shortage of 900,000 midwives, mostly in Africa: that’s one-third of the number of midwives required to meet global demand. It’s estimated that addressing this gap and fully investing in the global midwifery workforce would save 4.2 million lives each year, or around two-thirds of all maternal and neonatal deaths and stillbirths. Investing in midwives doesn’t just lead to positive health outcomes — it also contributes to building economies and achieving gender equality.
In Sierra Leone, midwives help facilitate safe and effective health care experiences, reaching the country’s most vulnerable mothers and building trust in health services. Banneh Daramy has been a state-certified midwife in Sierra Leone since 2015. In 2017, she became a newborn consultant for Project HOPE, and oversees our Kangaroo Mother Care (KMC) program and the facilitation of our mother care support groups.
Read on to learn more about what inspired her to enter the world of midwifery, the impacts of COVID-19, and what’s she’s focusing on in 2023.
What inspired you to become a midwife?
I decided I wanted to be a health worker after graduating from high school. I already had a passion for taking care of babies, and I wanted to save lives in my community. I was a community health nurse first. The maternal mortality rate at that time was so high. We went to a hospital in Freetown, and I saw a pregnant woman outside crying. I started asking her questions and she said she had been abandoned by her family because they didn’t have enough money for the prescription she needed. so I decided to help her. Since then, I’ve continued this passion for saving the lives of babies and their mothers. Seeing a baby for the first time, at birth, is really what inspires me most.

Midwives play a central role not only in maternity care, but across the entire continuum of sexual, reproductive, maternal, newborn and adolescent health care. Can you tell us a little bit about the different roles midwives play in your country?
We have a lot of different roles — we don’t just attend births. We are also counselors. Our customs and traditions here are different, especially with married couples. Pregnant women go through a lot, and as a midwife, we get close to their personal lives. Many women are afraid to talk to nurses, and we encourage them to share their issues and worries with us. We also take them through antenatal care. We started with eight required visits, but now we have women attending 16 visits before giving birth, and after delivery, we monitor and track their health.
In public hospitals, most patients are not literate, and many are very young — I’ve seen 13-, 14-, and 15-year-old pregnant adolescents. They don’t always know how to take care of themselves, but they are afraid to talk to people who are educated. Some are even scared to go to the hospital. Our approach automatically changes everything — we always lead with a smile when we first see a new patient. We smile and we welcome them. Then they feel more comfortable to talk to us, and they are more open to following our guidance and encouragement to go to the hospital.
Most of our patients come from very poor provinces. They don’t have enough food and they can’t afford prescriptions, so sometimes we even come together to help them. We don’t have to, but we want to see them healthy and we want them to be able to go home.

What was the most challenging part of your job during the COVID-19 pandemic?
Infection prevention and control. Many people do not practice handwashing, and it took a lot of energy and effort to handwash during COVID-19. Not everyone was able to wear a mask, and vaccines weren’t available at most hospitals and clinics. So even when people were COVID-positive, they didn’t go to the hospital.
Health services were largely disrupted for women and newborns at the peak of COVID-19. Everybody was afraid of each other. Nurses weren’t wearing masks, and patients weren’t wearing masks. We didn’t even have gloves in our offices. We don’t have much equipment or materials in our hospitals, so most times health workers were asking patients to buy their own personal protective equipment. As a result, most patients were neglected.
What role did you and your team play during the crisis? Did the pandemic lead to new ways of delivering services or providing education and training?
When COVID-19 started, we issued items to mothers in the communities through the mother care groups. We also talked to them about handwashing and the use of masks.
During the pandemic, Project HOPE volunteers also built Sierra Leone’s first undergraduate program in neonatal nursing and pediatrics in partnership with the College of Medicine and Health Science at the University of Sierra Leone. Most of the curriculum development and faculty training was done virtually, because of restrictions. And this month, we will be launching our country’s first advanced neonatal Master’s degree — a Master of Science degree in Neonatal Nursing.
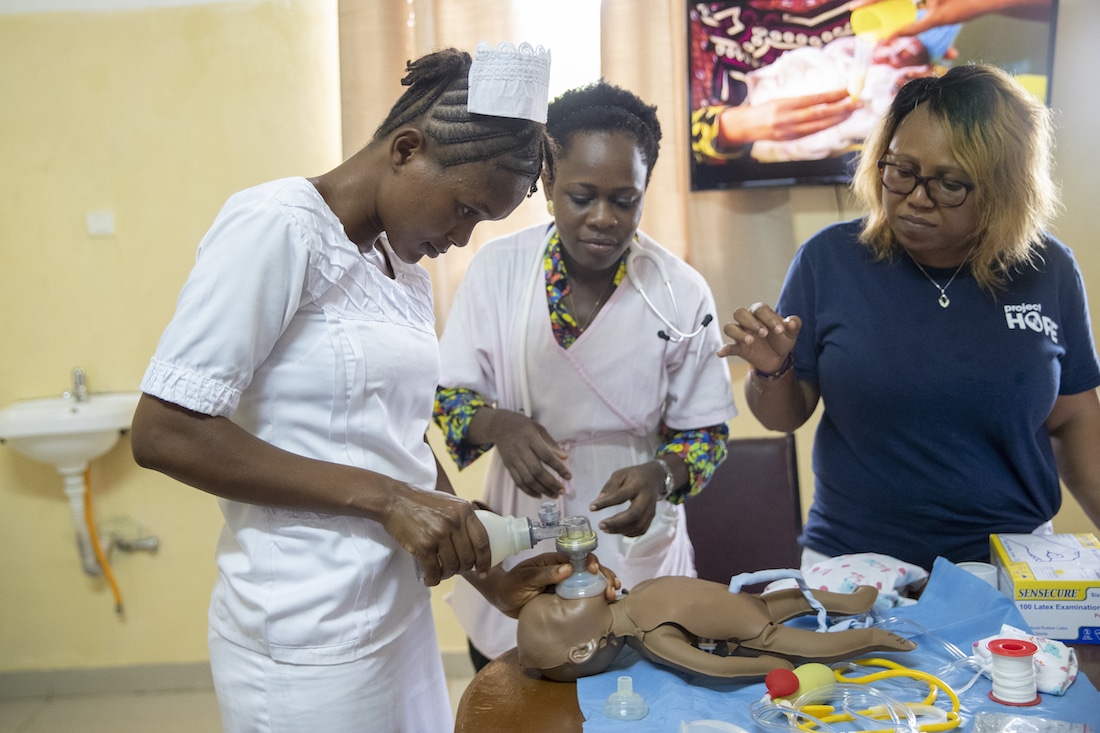
How serious is the shortage of midwives in Sierra Leone? What are some of the main reasons for the shortage?
There is a very critical shortage of nurses and midwives in Sierra Leone, which is why a lot of attention is being paid to training and educating new generations. We have three midwifery schools in different provinces of the country now — we used to have only one in Freetown. Soon we will have a fourth.
We’ve had a shortage because of the educational and training requirements. It’s difficult to become a midwife. You have to have three-to-five years of experience in nursing before you apply for midwifery. This year, since mortality rates are so high, they’ve started taking trainees directly from school, but they haven’t been accepting people from school level until now.
What’s the most rewarding part of your work?
The most rewarding part of my job is to see sick babies get better, get healthier, be discharged, go home, and come back for follow up.
I was the first nurse to start kangaroo mother care (KMC) in Sierra Leone, on the Project HOPE regimen. At that time, many preterm babies were dying. Then we started training people on KMC, and babies were surviving, getting discharged, and returning to the hospital for checkups healthy. Seeing this development is what I love most about this job. But I do this work for my country, not for myself. I do this work because it makes a difference. It’s not a job, it’s a passion. The assistance we provide benefits everyone. Saving one life goes a long way.

Sierra Leone has some of the world’s highest maternal and infant mortality rates. Has any progress been made over the past few years?
Yes, in spite of COVID-19, we are still making progress and reducing the risk of premature death, especially on the maternity side. We are a very poor country, with poor sanitation and nutrition, and women have not had good access to quality health services, but things are changing. Though the rates are still alarming, they are slowly improving.
I think this is thanks to having more midwives now and a lot of support with training, equipment, and volunteers from NGOs.
What are your hopes for 2023? What are you currently focused on, and what kind of progress would you like to see this year?
Through Project HOPE I want to continue with the training, especially on Helping Babies Breathe. Nurses and midwives are suffering. We don’t have anyone to talk to or cry to, but giving us more training helps fuel our passion for the job. As we attend more trainings, we see more and more of our patients discharged, and this success makes us feel more competent and secure.
We also need more equipment and training on how to use it. In some cases we have equipment but we don’t know how to use it, so it gets put aside.
I think it’s also important to focus on mothers just as much as babies. We need to do more training with mothers, and we need to teach nurses how to take care of the mothers too. We often put most of the focus on babies, but let’s see what difference we can make this way.

How you can help
Make a lifesaving gift to support our work now and for the future at projecthope.org/donateAre you a health-care or other professional who would like to learn more about volunteering abroad with Project HOPE? Learn more about our volunteer program and join our volunteer roster.
Stay up-to-date on this story and our lifesaving work around the world by following us on Facebook, Instagram, LinkedIn and Twitter, and help spread the word by sharing stories that move and inspire you.