
Q&A: Are Infectious Disease Epidemics Spiraling Out of Control?
Mpox, COVID-19, meningitis, polio — the list of infectious diseases seems to be increasing around the world. Is this a new threat to global health? What causes vaccine hesitation? And what role does misinformation play? Learn more in this Q&A with Project HOPE Chief Health Officer Dr. Tom Kenyon and Deputy Chief Health Officer Dr. Nagesh Borse.
In addition to Mpox, we’re reading more in the news about the spread of vaccine-preventable diseases like COVID-19, meningitis, diphtheria, and polio. Is this a new threat to global health? Or is the world just paying more attention?
Dr. Tom Kenyon, Chief Health Officer: A lot is going on at the moment, but outbreaks of vaccine-preventable diseases are definitely not a new concern. When I started with Project HOPE in the 1980s in Africa and the Caribbean, I saw many cases of whooping cough, congenital rubella, measles, meningitis, pneumonia, gastroenteritis, and neonatal tetanus. Many children died. But the World Health Organization, UNICEF, and partners led a highly successful “child survival revolution” where vaccines made a huge difference, helping to cut child mortality worldwide in half over the past 30 years. We have been very active with this. Though pockets remain, many vaccine-preventable diseases have largely disappeared and complacency is now a problem.
Simultaneously, a number of overlapping “disruptors” are driving vaccine coverage rates downward. That results in a growing number of people who are now susceptible to vaccine-preventable diseases. Ironically, according to the WHO, more people were vaccinated in 2021 (because of COVID-19) than at any time in our history, yet vaccine coverage in children has fallen back to 2008 levels. COVID-19, conflict, climate-related disasters, poverty, weak health systems, crowding, travel, and vaccine hesitancy have created the perfect storm. Increasing exposure to wild animals also increases the likelihood of new zoonotic diseases like COVID-19 and that is not likely to change anytime soon.
We’re in a red alert period and need to act collectively and urgently to raise vaccine coverage levels worldwide. We need to fund global health security with consistent reliable funding the same way we fund the Department of Defense to maintain national security against our enemies. We need to get out of the “panic and forget” mentality. The only alternative is continued devastation to society, insecurity, and trillions of dollars in additional losses to the global economy.
Uninterrupted funding for global disease detection and surveillance is so important … By the time you have a disease in New York City, it has gone everywhere.
Dr. Nagesh Borse, Deputy Chief Health Officer: I agree. When we talk about the importance of vaccinations, I think back to polio. If you go back, the investments that were made in vaccinating people against polio worldwide were because we knew the cost of vaccination worldwide is much lower than treating polio in the United States. We had an economic case for global vaccination campaigns. Now imagine doing it for all the diseases that are vaccine-preventable, whether you’re talking about polio, COVID-19, or HPV, which is not transmissible but can be prevented with a vaccine that is not available in many African countries.
Global disease surveillance is another issue that I feel is a missing piece now. Uninterrupted funding for global disease detection and surveillance is so important to detect diseases quickly in rural areas of countries where they may originate rather than trying to respond when they appear in the U.S. By the time you have a disease in New York City, it has gone everywhere. The countries that are good at surveillance are doing their own piece, but there’s no global coordination on it. Mpox is a good example. If we had good global disease surveillance and had invested in responding to mpox in endemic countries in West Africa, then it probably wouldn’t have transmitted globally. In the absence of those investments, now the U.S. has the highest number of mpox cases in the world.
Dr. Kenyon: We also have a serious issue with the capacity of the global health workforce. Before COVID, we were 18 million health workers short of what is needed for reaching the Sustainable Development Goals. We’re even further short of that number now. Global populations are growing and the ratio of health care workers to populations is going down. You need a health worker—including community health workers and stronger primary health care systems—to deliver a vaccine. Partnerships are critical because nobody can do it all.
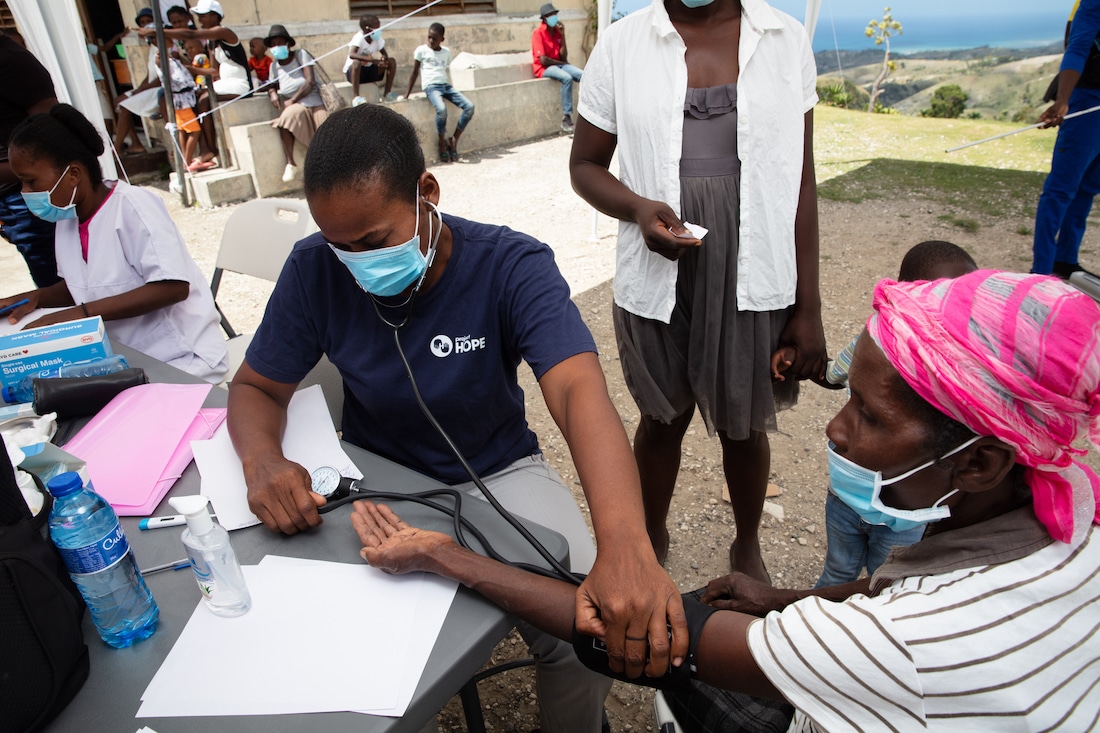
We’ve seen a rise in vaccine hesitancy in the U.S. during the pandemic. Is vaccine hesitancy an issue around the world, and what role does misinformation play?
Dr. Borse: I see vaccine hesitancy globally a bit different than in the U.S. In the U.S, misinformation plays a major role in vaccine hesitancy. People may just believe something is a fake disease. In the rest of the world, if you go to any country in Africa and go to the health facility in the morning, you’ll see the mothers lined up for their kids’ vaccinations. They’re walking miles to get there. That has not changed and I don’t think it will change.
The hesitation comes from—and this is also an issue in central Europe—that these are government-procured vaccines. The public trust in government-procured vaccines is one of the many reasons for their hesitation. Are they of good quality? Are they going to hurt my kids’ health? Sometimes there are vaccine side effects, or maybe there’s some kind of unrelated death after a child gets vaccinated. I was working for the WHO as a technical advisor in the Philippines when the measles vaccination stopped for a while because a child died after a vaccination, which was unrelated to the vaccination. When there are issues like that that are not completely understood by the community, that leads to vaccine hesitation.
Now, that was before social media. With social media, you also have an issue where if someone sees someone from an educated society in America saying a vaccine is not safe and they’re putting it out on Twitter, people around the world may start to believe there’s something wrong with it. Misinformation spreads quickly and widely. In 2020, the World Health Organization listed their 10 biggest threats to global health in the coming decade, and one of the 10 was the rise in vaccine hesitancy as misinformation brought on by social media and the anti-vaccination movement.
> LEARN MORE: How Vaccines Save Lives
Dr. Kenyon: Misinformation on vaccines needs to be addressed by leaders the community trusts. Yet in my experience, mothers in low- and middle-income countries have seen vaccine-preventable diseases kill their children and they mostly welcome vaccination. Project HOPE helped combat hesitancy through our COVID-19 vaccine trainings for health workers in Africa, Asia, and Latin America before the vaccines were even distributed. Health workers play a key role in educating their community and fellow health workers. We spent a lot of time sharing what the WHO was saying about the evidence for the many new COVID-19 vaccines.
It’s very important for countries to trust one another, which we see is lacking. With COVID, it has been everyone for themselves. The lack of global cohesion has limited progress. The WHO tried, but many countries did their own thing, often against WHO advice. So there’s a lot of diplomacy that has to take place. There’s plenty of work to do, and we’re only going to get more and more of these diseases, especially as the climate continues to warm. The problem is going to get worse as you get more crowding, as you get too much water or too little water. It’s going to affect so much: microorganisms, migration, poverty levels, the biosphere, you can go on and on. You’re never going to truly be able to predict what’s coming next. It’s so hard to predict. The better approach is to be prepared.

What should countries be doing to more proactively prepare for the spread of these diseases?
Dr. Kenyon: The Global Health Security Agenda was launched in early 2014 by former U.S. Secretary of Health and Human Services Kathleen Sebelius and the Director General of WHO Margaret Chan, and the point was to galvanize the global community around a collaborative approach to pandemic preparedness and response. The GHSA outlined the very specific skills and capabilities a country should have to detect and deal with disease outbreaks so they don’t expand into large-scale epidemics and pandemics. So the framework is there and it is more a matter of global implementation and long-term investment.
For the U.S. specifically, we did a lot of work when I was at the CDC during the 2014-15 Ebola outbreak in West Africa to develop the interagency playbook for pandemic preparedness and response. We worked with numerous countries and the WHO to strengthen public health systems and helped to launch the Africa CDC. The White House provided important leadership, visibility, and mobilization of resources, including short-term one-time funding from Congress and logistical support from the Department of Defense for the first time. The interagency roles became clarified recognizing USAID as our international development agency, CDC as our public health agency, NIH for the development of new technologies, and the Department of State for the diplomatic aspect.
> LEARN MORE: How Project HOPE Supports the Global Health Security Agenda
But the political platform of the White House is not the right environment from which to actually fight a pandemic. The playbook didn’t survive the transition from one administration to the next for political reasons. We wouldn’t fight a war that way and we shouldn’t fight pandemics that way. Funding to build public health capacity also can’t be short-term as happened following Ebola because we know it takes decades of effort to develop public health competencies.
Ultimately, the fundamental issue in slowing vaccine-preventable diseases is achieving and maintaining equity as our guiding principle. These diseases simply cannot be contained unless there is equity across nations and across vulnerable populations within those nations. Vaccine equity is a moral imperative and in our own self-interests. Ultimately, vaccine-preventable diseases will reach the reservoir of susceptible people no matter which country they come from, as we’re seeing today with COVID-19, measles, and polio. And the return on investment in vaccines is extraordinary.
What role does stigma play in the spread of infectious diseases, and how can health systems work to overcome it?
Dr. Kenyon: Stigma is almost inevitable with infectious diseases and can originate from within the individual, from within the health system, and from the community. I see it as a workforce solution. One way organizations like Project HOPE can help is by building a country’s capacity to communicate. Communication is highly cultural, and countries are very adept at communicating with their culture. In Ethiopia, you have over 200 different languages and very different cultures. You have to tailor communications to each population. That’s why in a national immunization program, you should have a communications person on the team. They’re as much a part of the team as a nurse or a cold chain technician.
We just need to anticipate that stigma is going to be there and address it head-on with consistency and with the truth. Social media is uncontrollable, so you have to control your own messaging and get the truth out. You can’t go wrong in just communicating what you know and reassuring the public what we don’t know but are working on.
Usually, stigma comes early in an epidemic when we don’t fully understand modes of transmission and people develop their own ideas about how a disease is transmitted. That was an issue early on with HIV in Africa. It has been a major issue with COVID-19 and is happening now with mpox. When you get into these corners, you have to find a communications way out of it. That’s why having a strong local workforce is so important. Our Ebola response was eventually successful because the information got down to the village level, where a lot of misinformation was coming from. You have to get that right.

Usually, stigma comes early in an epidemic when we don’t fully understand modes of transmission and people develop their own ideas about how a disease is transmitted. … When you get into these corners, you have to find a communications way out of it. That’s why having a strong local workforce is so important.

Dr. Borse: There’s also a lesson we can learn from how the rest of the world has overcome hurdles in getting polio vaccinations in vaccine-hesitant communities. In Nigeria, you had religious leaders and village leaders taking part in polio vaccinations so there was no hesitation in the community. In India, a Muslim Bollywood actor would come out publicly talking about the safety of the polio vaccine. There’s room for U.S. health care systems to think about who those community champions are in those communities that can be included in these discussions. How do you bring a non-health champion to talk about vaccines?
Another area that can be further invested in is adulthood vaccination, which is non-existent in the rest of the world. Vaccination is only associated with children and there are no adulthood vaccinations.
COVID-19 was a big learning for adulthood vaccinations in the rest of the world. I was amazed by the number of adults who got vaccinated against COVID-19. That’s a new platform we have now that can be leveraged for other vaccine-preventable diseases. It’s been a blessing in disguise that we have that adult vaccination platform. Now, how can we use it?
How you can help
Make a lifesaving gift to support our work now and for the future at projecthope.org/donate
Are you a health-care or other professional who would like to learn more about volunteering abroad with Project HOPE? Learn more about our volunteer program and join our volunteer roster.
Stay up-to-date on this story and our lifesaving work around the world by following us on Facebook, Instagram, LinkedIn and Twitter, and help spread the word by sharing stories that move and inspire you.