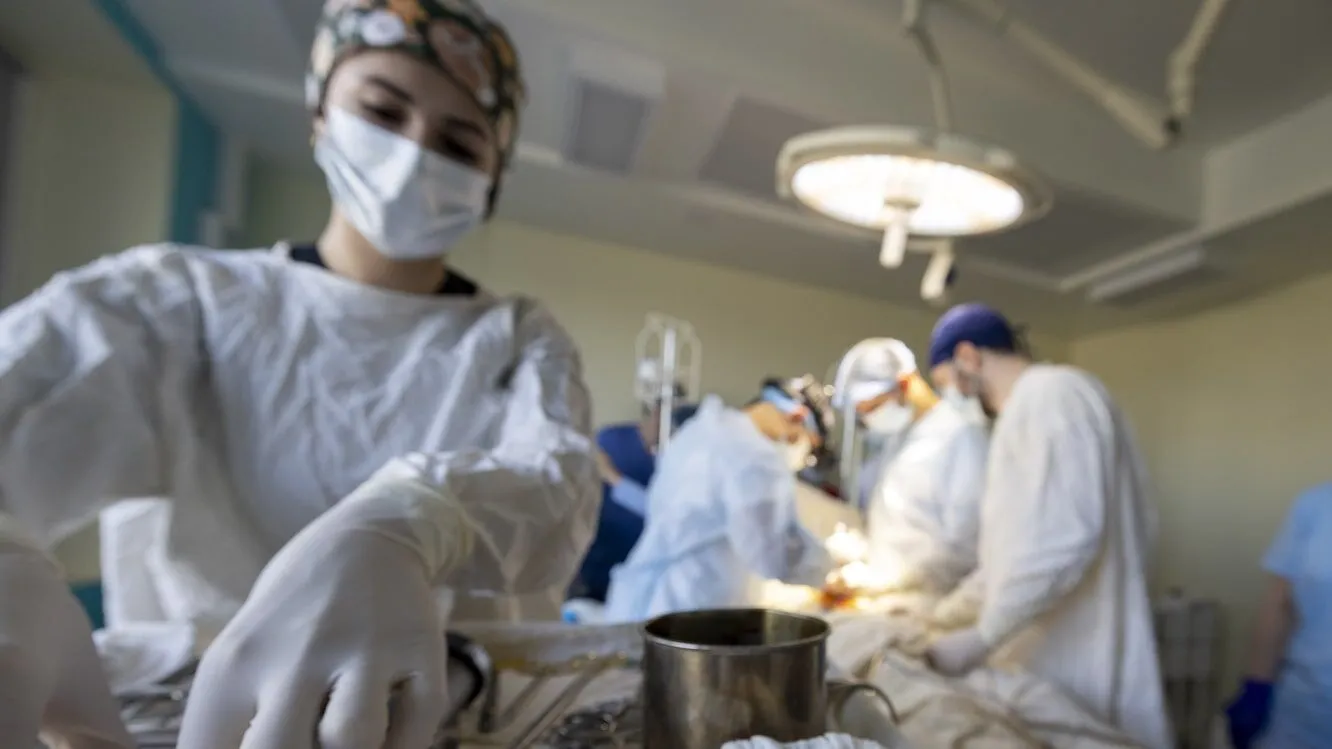
In Sierra Leone, Health Workers Spark Long-Term Transformation
Project HOPE is working across the health system in Sierra Leone to build long-term solutions for mothers, infants, and health workers determined to lower the country’s high rates of maternal and neonatal mortality.

When Aisha was born, the odds were stacked against her.
Born two months early, she was dangerously underweight—only three pounds at birth. Any disease would likely prove fatal. And in Sierra Leone, where Aisha and her mother Khadija call home, 1-in-10 children don’t make it to their fifth birthday.
Aisha was admitted to the Special Care Baby Unit (SCBU), a critical care ward Project HOPE supports at Ola During Children’s Hospital in Freetown. In a country with some of the highest neonatal mortality rates on earth, the babies inside the SCBU are among the most serious. Doctors and nurses at the SCBU care for more than 250 newborn children like Aisha every month, rushing from infant to infant, many of whom are on oxygen or fighting deadly infections like sepsis.
Khadija, 29, who was recovering from an emergency C-section after experiencing pre-eclampsia, had not seen her daughter after she was taken to the unit.
“I was scared,” she says. “The first day I was discharged from my ward to see my baby I was so nervous to go to her. It was not easy for me in those moments. It was very emotional for me.”
After three weeks in the SCBU, Aisha’s weight increased to 3.7 pounds, a small but critical milestone that showed she could be moved to the Kangaroo Care Unit Project HOPE established nearby, where nurses helped Khadija nurse and hold her daughter skin-to-skin. Before long, Aisha had gained enough weight to be discharged.
One year later, Aisha is small but strong: 11 pounds, with no complications. At a follow-up appointment back at the SCBU, Aisha takes some of her first wobbly but determined steps around the ward.
“I have so many dreams for her,” Khadija says. “I want her to be a doctor in the future. I want her to save babies just like she was.”

Sierra Leone has made great progress in maternal and neonatal mortality, despite recurring shocks to its health system like the 11-year civil war and 2014 Ebola epidemic, which killed a staggering 21% of the country’s entire health workforce. When Aisha’s mom was born in 1995, the under-5 mortality rate was 1-in-4. Yet, health workers struggle with dangerous shortages of basic medicines, medical equipment, and trainings that have made achieving long-term transformation difficult.
Project HOPE is working across Sierra Leone’s health system to equip the doctors, nurses, and midwives who are determined to change the narrative. Project HOPE has sent rotations of medical volunteers to the SCBU to train doctors and nurses on equipment, improve their charting system, and even develop a drug reference book for all medicines used in the ward. Project HOPE’s biomedical engineer volunteers have worked with the hospital’s maintenance staff to repair critical equipment like oxygen machines and CPAP machines that are used in the ward. Thirty nurses in the unit recently attended a Helping Babies Breathe training on infant resuscitation. This year, Project HOPE is repairing the water tank so the SCBU will have clean water again.
But long-term impact in Sierra Leone also means strengthening the outlying rural clinics and community health centers that are forced to refer babies due to dangerous shortages of basic medicines, medical supplies, and equipment.
Esther, a nurse in a rural village called Campbell Town, delivers about 30 babies every month in the small concrete delivery room at her clinic. Mothers can only stay four hours after delivery before they are discharged. If it is an emergency—if they are bleeding, or if the baby must be delivered via C-section—they must find transportation for the long ride to the hospital, which might mean riding on the back of a motorbike. The lead mother in Campbell Town plays a vital role in visiting new mothers in their homes throughout pregnancy and delivery to ensure they are exclusively breastfeeding their children and receiving all necessary vaccinations.
“In this community there are a lot of first-time mothers,” Esther says. “Most of them are teenagers. Some are as young as 14. Some of them are afraid to come to the clinic because of the stigma. We encourage them. With the help of the lead mothers, they go out and talk to them and bring them to the hospital.”
In January 2024, Project HOPE hosted a Helping Babies Breathe training for midwives across the area, led by volunteers from Latter-day Saint Charities. The trainings covered essential skills to help resuscitate newborns and provide postnatal care that ensures babies can survive.
About 30 midwives attended the training, including many from small rural clinics like Esther’s and outlying hospitals. These lead trainers will now cascade what they learned to 150 more midwives across the region, equipping the country’s workforce with the skills they need to save thousands of newborn lives.



Back at the SCBU, lead nurse Hawa walks from newborn to newborn, checking vitals, meeting with care nurses, and orchestrating the frenzied stream of activity that keeps the babies alive.
Hawa has worked in the SCBU for 10 years, enough time to see first-hand how the level of care has risen for the delicate patients in her charge.
“We’ve seen improvements in patient care,” she says.
“The other nurses say that being posted here is a punishment. They say, ‘What have you done? You were posted to a punishment.’ Because the work is very hard. But the patient care here has really improved. Now we can properly assess babies. When babies come in, we get their vitals and their weight. The unit is much quieter now. I enjoy working here.”
Hawa has also seen the landscape change for Sierra Leone’s health workers. The Ebola epidemic was a tragic reminder how fragile, yet critical the workforce is. But since then, the career has become more respected, salaries have risen, and more people are interested in becoming health workers.
Thanks to Project HOPE, they now have the opportunity. At night, Hawa attends classes at the graduate program in neonatal nursing that Project HOPE established in partnership with Jefferson College of Nursing and the College of Medicine and Allied Health Science in Sierra Leone. Hawa received her Bachelor of Science in Pediatric and Neonatal Nursing in the program before enrolling to receive her Master of Science in Neonatal Nursing. When she graduates, she can apply to be the lead nursing officer at the SCBU.


The growth of the program reflects the changing attitude toward health workers in Sierra Leone, says James, a Project HOPE fellow who teaches Hawa and other students in the school. The first cohort had 11 graduates; the second, 13. The third cohort that will graduate in April 2024 will have 45.
“This is the first-of-its-kind national program,” James says. “When I’m teaching, I learn at the same time. The fellowship program is a good initiative by Project HOPE. It’s a learning ground for us.
“I believe if we continue to have more graduates, more fellows, we can reduce our neonatal mortality. In the last two or three years, the statistics have started to go down. Kudos to Project HOPE. Being a fellow to me is a benefit to my credentials, it’s a benefit to our country, it’s a benefit to the university. Education matters.”