Ghana’s Health Workforce is Shrinking. These Midwives Are Feeling the Fallout.
Midwives and nurses in Ghana share how the large-scale departure of health workers is impacting their day-to-day work, and why they’ve decided to stay.
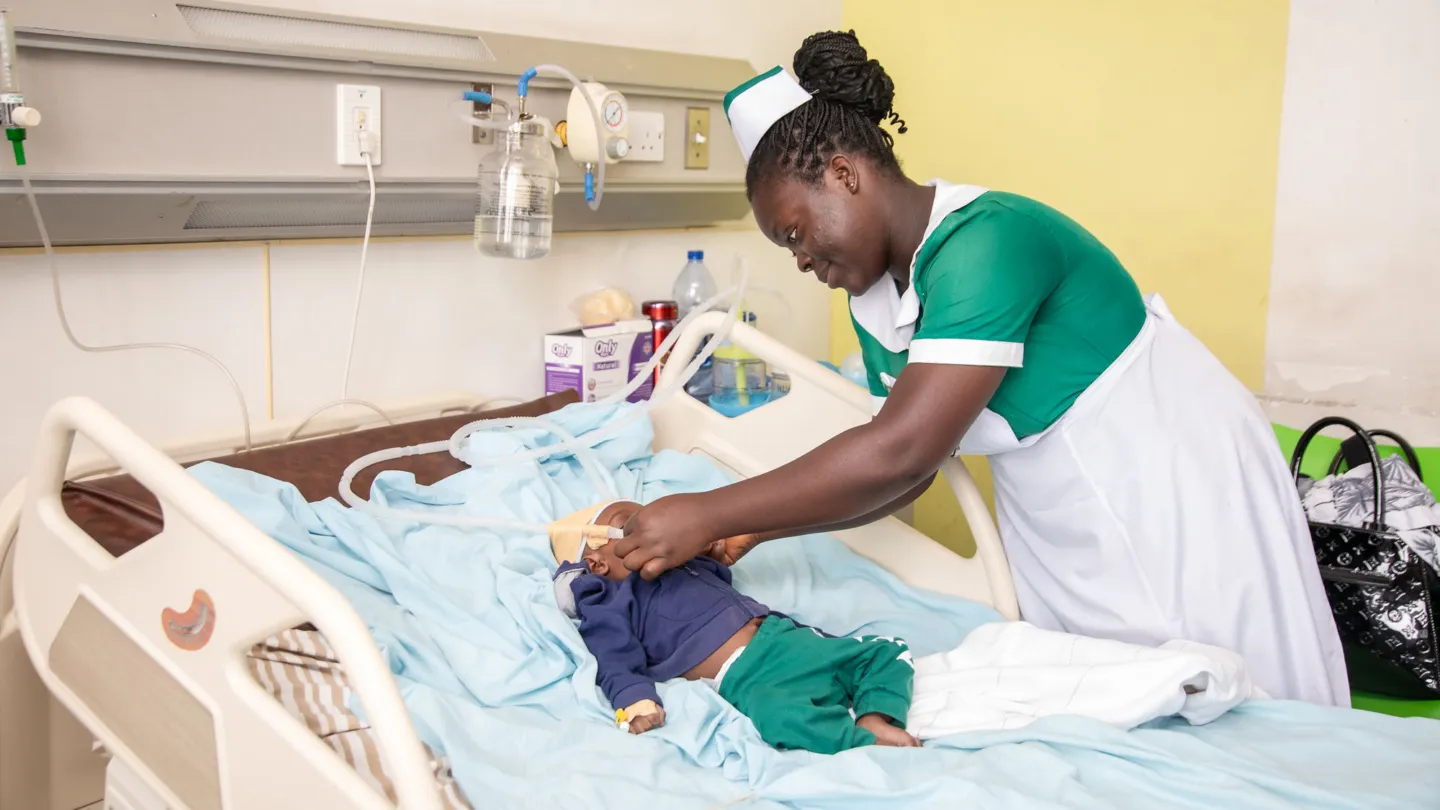
Across Ghana, health workers are being asked to do more with less.
More than 3,000 nurses and midwives are estimated to be leaving each year seeking better pay and working conditions abroad, part of a widening exodus that has been reshaping the country’s health system since COVID-19. The trend shows no signs of slowing. In a 2025 study, nearly 70% of surveyed Ghanian health workers said they intended to migrate within the next five years, including 85% of doctors, 72% of nurses, and 63% of midwives.
The situation is especially alarming in the northern part of the country, where around 1 in 5 children are chronically malnourished and over half of primary health facilities already lack basic infrastructure and essential medical equipment.
Project HOPE is working closely with remaining health workers to improve health outcomes for mothers and babies. Five of them explain what it’s like to work in a system under growing strain, how the shortage impacts their day-to-day work, and why they are choosing to stay.

Kuusuo Matilda Gangana, midwife at St. Joseph’s Hospital in Jirapa
I have been a midwife in northern Ghana for 11 years, and from where I stand, the health system is under significant strain. We have too few health workers serving a growing number of patients, and staffing is uneven — urban areas tend to have more personnel, while rural areas have far fewer. At the same time, many experienced professionals are leaving, placing even more pressure on those of us who remain.
In my daily work, it means fewer hands and more patients. The workload becomes overwhelming, which leads to delays in attending to emergencies, long waiting times, and limited time to assess and treat patients or properly consult and explain procedures. It also affects our own health — stress and fatigue are constant.
I care for pregnant women, newborns, and mothers in the postnatal period.
When we are overstretched, mistakes are more likely. Monitoring can be inconsistent, increasing the risk of infections and complications, and recovery can be slower. In some cases, the cost of care increases. We lack some essential staff, such as a gynecologist, and at times, motivation can be difficult.
I stay because there is a deep sense of purpose in this work and in helping patients recover. I remember a young boy who had fallen from a tricycle and suffered severe wounds. His parents could not afford continued care, so I used supplies from my own first aid box to dress his wounds and encouraged them to seek further treatment. They followed my advice, and within a week, he recovered. Moments like that keep me going.
Health workers are human. We get tired. We have emotions. We carry a lot of responsibility. But with the right support — most importantly adequate staffing, a safe working environment, equipment, and training — the entire health system can improve.
I stay because there is a deep sense of purpose in this work and in helping patients recover.

Monica Quainoo, midwife & clinical mentor in Jirapa and Lawra
I work as a clinical mentor with Project HOPE, supporting health workers who care for mothers, newborns, and children in Jirapa and Lawra. Through hands-on coaching, simulations, and real case support, I help midwives strengthen their skills and improve service delivery.
The work is demanding. We face shortages of equipment and essential medicines, and when health workers are overstretched, patients may not receive the full attention they need. Staff shortages compromise quality, safety, and timeliness of care, leading to delays, lapses in monitoring, and over time, burnout.
I have thought about leaving, but I have chosen to stay. I am following my passion to serve my own country. What inspires me to keep going on difficult days is knowing that my efforts can directly impact someone’s life. Even small actions, mentoring a colleague, improving a facility, or ensuring a safe delivery, can make a difference.
I’ve also seen what’s possible. I once led the conversion of a veranda into a delivery room, allowing a facility to conduct its first childbirth safely. That moment showed me that even small, practical innovations can expand access and save lives.
Health workers are the backbone of health care, yet their sacrifices often go unnoticed. Investing in our training, safety, and well-being is essential for the millions of people who depend on us.
Investing in our training, safety, and well-being is essential for the millions of people who depend on us.
Naanyere Portia, midwife at St. Joseph’s Hospital in Jirapa
Ghana’s health system is characterized by inadequate staffing and the uneven distribution of health workers. Many nurses and midwives are leaving the country to seek greener pastures, and even doctors sometimes refuse postings to regions like ours.
For those of us who remain, the work meant for many is being done by only a few. It is stressful and worrying. I have been a midwife in Jirapa for seven years. We care for women before, during, and after pregnancy, as well as newborns, but we need better working conditions and lack critical resources — an obstetric theatre near the maternity unity, functional vacuum machines, a rotational tool for suturing, and enough staff.
I have thought about leaving, but I have chosen my patients over financial gain and personal comfort. When colleagues leave, it hurts, and it increases the burden on those of us still here.
I am a mentee of Project HOPE, and the support has been very impactful. It has enabled me to provide quality care to my patients and go home satisfied after work. There are many key moments that remind me why this work matters. One day, a mother showed me her child, whom I had delivered years before, and said, “This is the midwife who delivered you.” That moment made me proud. Midwives save lives.
I have thought about leaving, but I have chosen my patients over financial gain and personal comfort. When colleagues leave, it hurts, and it increases the burden on those of us still here.
Tampah Felicia, midwife at Tizza Health Center in Jirapa
I have worked in Ghana’s health system for 16 years, starting as a community health nurse and now serving as a midwife at Tizza Health Center in the Upper West Region. Across the systems, there is a shortage of staff in all categories, and poor distribution affects rural areas the most.
In my day-to-day work, the shortage places a lot of stress on health workers and makes it difficult to provide adequate care. I care for women through every stage — preconception, pregnancy, labor, delivery, and the puerperium — but we face inadequate staffing and a lack of logistics to support our work.
When health workers are overstretched, patients may be neglected, care may be delayed, or the care provided may be inadequate. The departure of colleagues only increases the workload and stress on those who remain.
Still, I have never thought about leaving. I chose to stay because of my love for serving my country. My mother taught me that once you make a choice, you must be responsible for it — and since I chose to become a midwife, I remain committed, even during difficult times.
What I love most is being able to provide the best possible care for my clients. Health workers genuinely care. We want the best for every patient. But we need better support: improved infrastructure, adequate logistics, opportunities for advanced training, and inclusion in decision-making, especially for those of us working in rural areas.
Because when health workers are supported, we can thrive, and so can the communities we serve.
Still, I have never thought about leaving. I chose to stay because of my love for serving my country.

Rebecca Manu, neonatal nurse at Kumasi South Hospital in Asokwa
I have been a neonatal nurse specialist in Ghana for 15 years, providing care to patients in my assigned department and supporting overall health care delivery in Kumasi South Hospital. I have been trained on essential newborn care by Project HOPE and provide cascade training to other health workers in my region.
While there has been improvement in infrastructure and service delivery, the number of trained health professionals is not keeping pace with the growing patient population. Many facilities, including mine, operate with fewer staff than required, affecting both efficiency and quality of care.
On a daily basis, we manage a high number of patients with limited staff, often taking on multiple roles, working long hours, and getting minimal rest. I care for some of the most vulnerable patients — newborns, mothers, and children, and individuals with chronic conditions like hypertension or diabetes — and when staffing is low, it can compromise safety, reduce time with each patient, and delay critical interventions.
I’ve considered leaving, like many others, but I stay because of my commitment to serving my community and making a difference. Seeing a critically ill patient recover and express gratitude reminds me why this work matters.
Behind every service provided is a dedicated professional working under pressure, often sacrificing personal time and comfort. Supporting them means strengthening health care delivery and saving lives.
I stay because of my commitment to serving my community and making a difference. Seeing a critically ill patient recover and express gratitude reminds me why this work matters.



