5 Things to Know About Health Worker Burnout
Around the world, high rates of burnout are driving health workers away from their work. Learn more about the burden health workers carry, why many keep silent, and the implications for patient care.
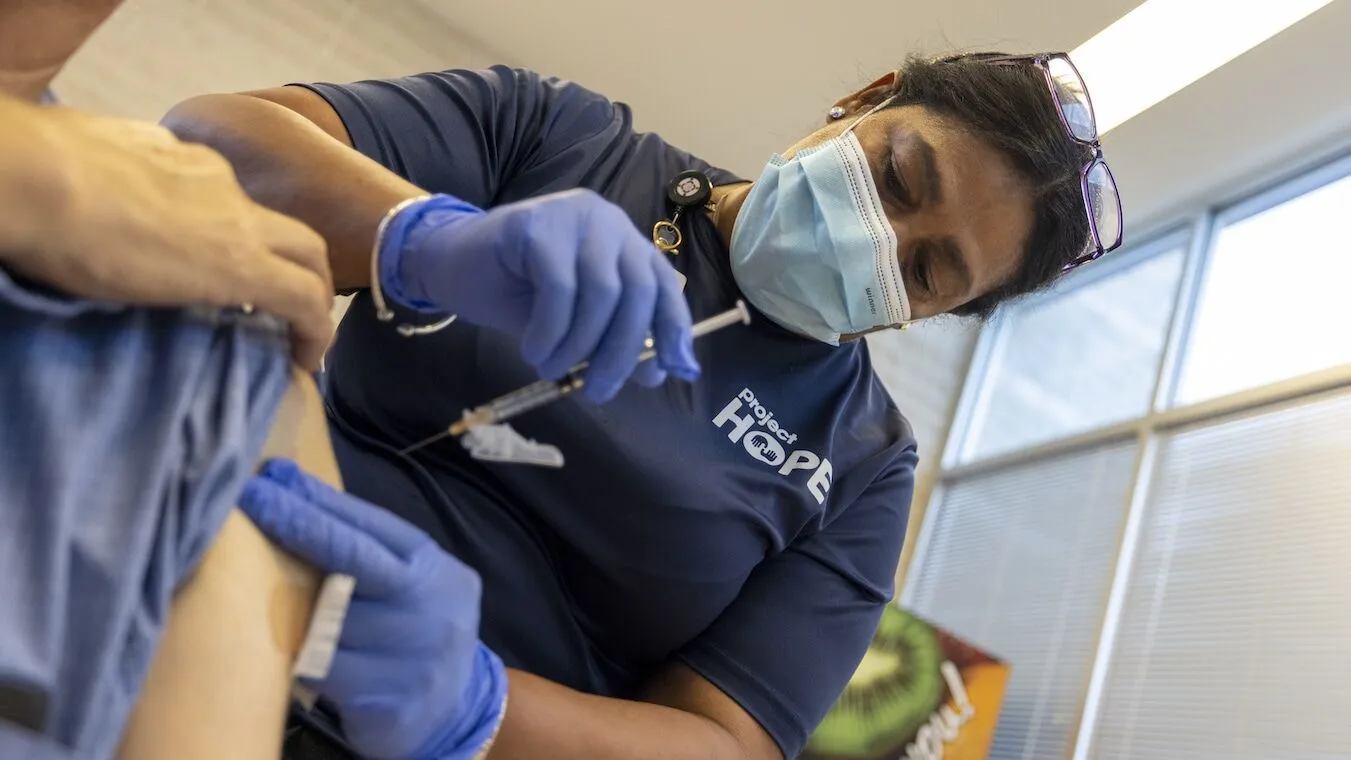
The world is suffering a significant health worker shortage, and burnout trends threaten to deepen the crisis.
The global shortfall is projected to reach 11 million by 2030, with burnout and mental health challenges serving as major drivers of workforce attrition.
Here are five things to know about health worker burnout and the impact it has on patient care.
1. Health workers are experiencing sustained burnout from COVID-19.
At least one-quarter of health workers reported symptoms of burnout during the COVID-19 pandemic. Though rates of burnout have eased slightly since peak pandemic levels, they remain persistently high as a result of staffing shortages, workload, and system pressures, with around one-third or more health workers continuing to experience burnout globally.
In the U.S. a recent survey found over half of U.S. health workers stressed, overworked, and ready to leave their jobs. Nurses report some of the highest levels of burnout.
2. Nearly one-third of clinicians are considering leaving their job or migrating in the next few years.
In a global survey of clinicians, 31% reported they were planning to leave their current role in the next two to three years, with even higher intent in some regions, including the Middle East and Africa.
About 33% of those considering a change said they would stay in the health care sector but pursue jobs in different settings. According to the World Health Organization, health workers are increasingly leaving lower-income countries for better opportunities abroad — a trend that continues to accelerate, exacerbating staff shortages in countries where resources are more limited and health challenges are most dire.
3. In the U.S., 1 in 5 health workers have quit their jobs since 2020, and more than half of health workers are considering changing jobs within the next year.
Burnout and mental health challenges affect health workers in countries around the world, including the U.S.
Nearly 1 in 5 U.S. health workers left their jobs during the COVID-19 pandemic, and about 4 in 5 health workers left behind say they’ve been affected by staffing shortages, working longer hours and with higher patient loads to compensate for fewer teammates.
The trend isn’t slowing down. Recent data suggests the crisis may be deepening: more than half of U.S. health workers (55%) say they plan to look for or switch jobs within the next year, with some considering temporary assignments in order to avoid burnout. Staffing agencies are reporting more interest in short-term travel assignments, which typically offer better pay and greater flexibility.
4. Health workers experiencing mental health challenges are likely to stay silent.
When health workers face mental health challenges, they often struggle to seek out treatment and support. Lack of mental health resources is a barrier, but social stigma and fear of professional reprisal are often the greatest impediments to care.
Although more than half of the U.S. health workers report experiences of burnout, anxiety, or depression, many refrain from seeking formal mental health support. Physicians are some of the least likely to seek help.
In a 2024 survey, around 77% of U.S. physicians reported stigma around seeking mental health care, and about 4 in 10 U.S. physicians shared that either they or a colleague had been afraid of seeking treatment because of confidentiality issues and concern that it would negatively impact their career.
To help reduce stigma and normalize mental health support, Project HOPE launched mental health and resiliency trainings for front line health workers under increased stress. These trainings bring health workers together to talk openly about topics like burnout, exhaustion, and compassion fatigue and to work through ways to combat mental health stigma in the workplace.

5. Burnout jeopardizes patient safety and care.
When health workers feel overwhelmed and experience burnout, it’s likely to compromise their ability to provide quality patient care. Studies link burnout to “suboptimal” practices and predict it to double the risk of medical error.
Burnout has become one of the leading causes of the global exodus from the health workforce, underscoring the urgent need to prioritize and expand support, including mental health, for health workers.
Around the world, we’re ensuring health workers have the support they need to protect their own health and well-being so they can sustain their livelihoods providing care for others.
This story has been updated from a previous article published on June 1, 2023.



