The Ripple Effects of Vaccine Regression
Global vaccine rates are falling. The consequences will be serious, far-reaching, and deadly.
For decades, strong immunization programs have reduced illness, disability, and death. But that progress is now at risk. Global vaccination coverage has declined in recent years, in large part due to the COVID-19 pandemic, and in many places, including the U.S., rates have yet to return to what they were before 2020.
This backslide is already resulting in serious consequences, triggering outbreaks of preventable diseases like measles and polio, straining health care systems, driving up health care costs, and threatening lives. And children under 5 are the most vulnerable.
The ripple effects of vaccine regression include outbreaks of preventable diseases, strained health care systems, higher health care costs, and life-threatening illnesses.
Measles is a dangerous example of these ripple effects, particularly in communities with declining vaccination coverage. There were an estimated 10.3 million measles cases globally in 2023 — a 20% surge from 2022 — largely driven by children missing one or both doses of the measles vaccine amid gaps in routine immunization coverage worldwide.
It’s likely that the upward trend has continued into 2024 and 2025.
Around 280,000 kindergarten children in the U.S. were unvaccinated and unprotected against measles last year. The result? A nationwide outbreak in March and the first U.S. deaths from measles in a decade. The number of national cases has now risen to the highest levels in over 30 years. More than 1,300 measles cases have been confirmed across nearly 40 states so far in 2025. Nearly 30% of those cases are among children, many of whom caught the disease overseas — a reminder that infectious diseases know no borders. In our increasingly interconnected and mobile world, under-immunization anywhere is a threat to global health security.
What is measles?
Until March 2025, measles was considered eradicated in the U.S., thanks to the success of the measles, mumps, and rubella (MMR) vaccine. But in 2024, the Centers for Disease Control and Prevention (CDC) found a decline in the number of kindergarteners that had received all state-required vaccines. This spring’s nationwide measles outbreak was the tragic result.
The majority of infections have occurred among unvaccinated individuals in communities where rates have dropped below the 95% threshold needed for herd immunity. More than 1,300 cases have been reported, and three people have died: an adult in New Mexico and two elementary school-aged children in Texas. These are the first recorded measles deaths in the U.S. in a decade. None of the three were vaccinated.
Measles is more serious than a short-lived rash and a high fever — it’s one of the most dangerous vaccine-preventable diseases, especially for children. Even when children recover, the effects can be devastating. Measles can cause brain damage and developmental disabilities, derailing a child’s ability to learn and thrive. It can also erase their immunity to other life-threatening diseases like pneumonia and RSV, leaving them more vulnerable to future infections.
In some cases, complications ripple across a lifetime, including heart murmurs, meningitis, encephalitis, deafness, and blindness. The impact of the illness extends beyond physical health — it can limit educational and career opportunities, disrupt daily hobbies and joys, and forever diminish a person’s full potential from a young age. The best protection against the infection and its ripple effects? The MMR vaccine.
The rise in cases of measles and other preventable diseases is not just a public health concern, but also a growing burden on the health care system.
Nearly 13% of U.S. measles infections this year have resulted in hospitalization, stretching already limited resources and diverting attention from other essential services. Treating preventable diseases comes at a steep financial cost as well. According to the CDC, every $1 spent on immunization in low- and middle-income countries saves $52, while the cost to fully immunize a child is only $18 in low-income countries.
Every $1 spent on immunization in low- and middle-income countries saves $52.

Most tragically, a decline in immunization rates costs lives.
Because of America’s recent decision to withdraw from Gavi, the Vaccine Alliance, more than 1 million children will die. Another 75 million will not get vaccinated. Since its founding in 2000, Gavi has helped vaccinate more than half the world’s children, with the U.S. serving as a major donor — pledging $2.6 billion through 2030 before terminating support in June.
Halting support at this stage presents great risks: reversing decades of progress against vaccine-preventable diseases, increasing the number of zero-dose children, and placing additional strain on already-overburdened health systems.
Project HOPE is committed to supplying health workers with the tools and support they need to address the health challenges they face — and improving access to vaccines has been an essential part of this work.
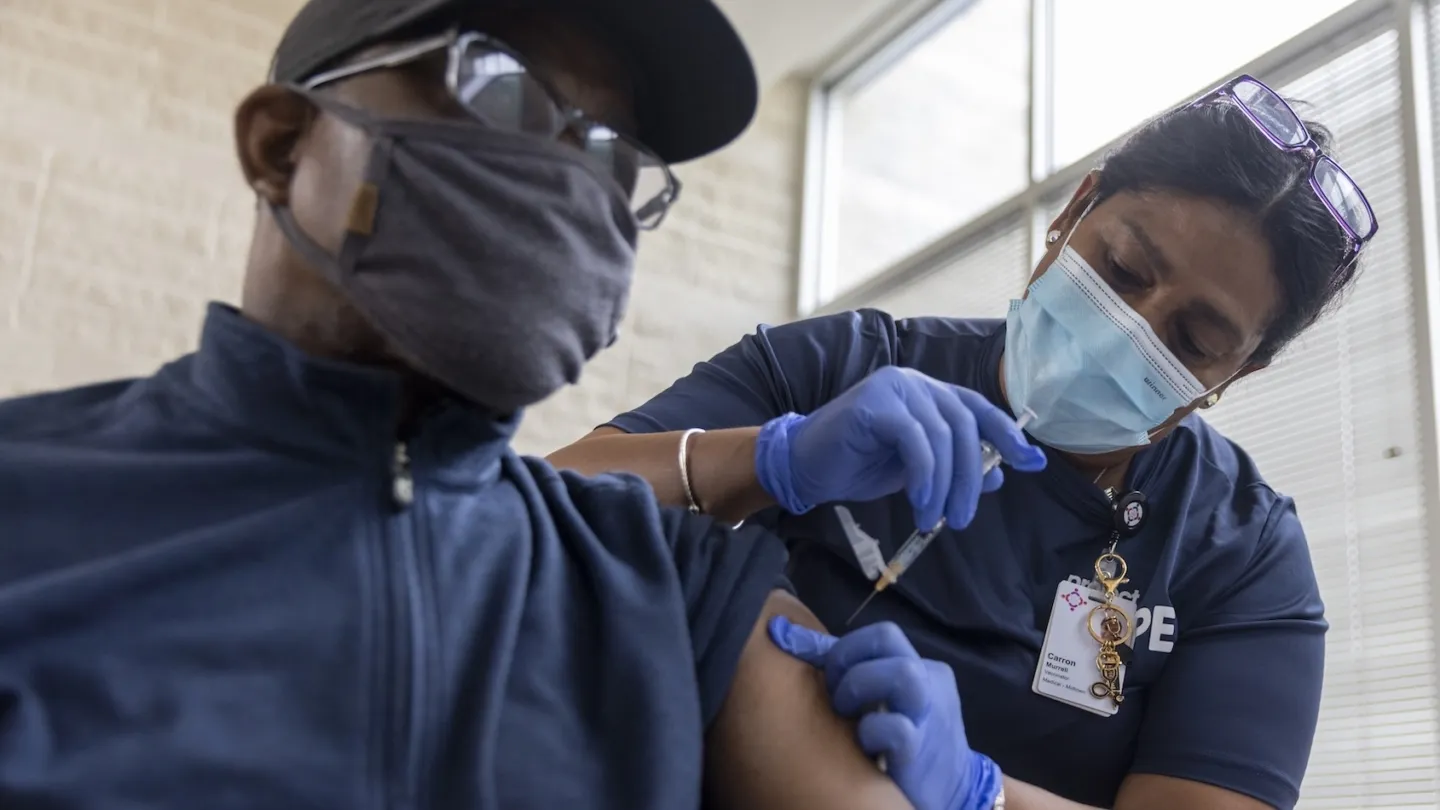
In the U.S., we’ve partnered with Moderna to provide thousands of COVID-19 vaccinations to free and charitable clinics across 30 states. Globally, we’ve delivered polio vaccines to children in Gaza and provided emergency immunizations — including polio — to displaced communities in Ethiopia. In Mozambique, we distributed cholera vaccines to high-risk populations following Cyclone Idai in 2019, and in the Dominican Republic, we’ve worked through public health clinics to reach families in remote areas.
As the immunization gaps widen, Project HOPE remains steadfast in equipping local partners with the vaccines and resources they need to protect communities across the country and around the world.



